Trauma
Bone and joint trauma, such as fractures and dislocations, are common and vary in severity from single fractures to multiple, life-threatening musculoskeletal injuries.
The most clinically challenging of these for the surgeon, and those that have the most socioeconomic burden, are open fractures. These often involve damage to the surrounding soft tissue, resulting in complications such as tissue and deep bone infection or long-term non-union.
Trauma has a significant and ever increasing impact on healthcare systems:
- In the EU, 5.3 million people are admitted to hospital as a result of accident or violence-related injury.1
- In the USA, there are over 41 million emergency department visits and 2.3 million hospital admissions.2
- In the EU, €80 billion per year is the estimated cost of injuries treated in hospitals (inpatients and ambulatory care).1
- In the USA, trauma has an estimated economic burden of $671 billion a year, including both healthcare costs and lost productivity.2
Injuries attending Emergency Departments in EU.1
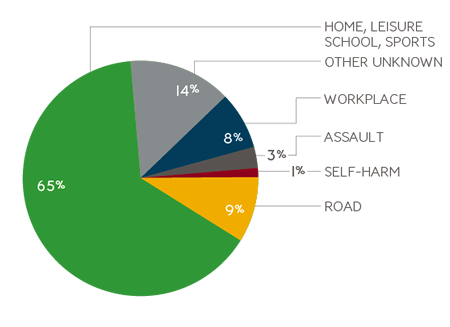
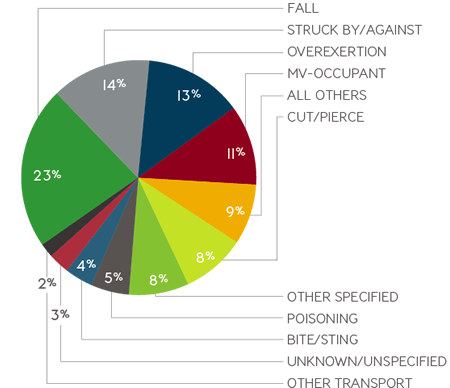
Leading causes of non-fatal unintentional injuries (age 15-65), in USA.3
Currently the gold standard for bone grafting is utilising the patient’s own bone. However, iliac crest bone grafts are often in limited supply and also carry attendant risks such as:
- Donor site morbidity
- Increased risk of infection due to a second surgical site
- Increased health economics
The use of effective synthetic calcium-based bone void fillers reduce a surgeon’s reliance on iliac crest bone graft, with ideal grafts having characteristics such as:
- Biocompatible
- Osteoconductive with a matrix allowing bone ingrowth
- Physiological pH
- Hydrophilic
- Truly absorbable at an optimal rate
- Controlled purity
- Low levels of drainage
Biocomposites has pioneered the development of calcium-based composite materials with improved mechanical properties, to give support during the healing period, to offer improved biocompatibility during absorption and to allow healing by bony growth.